What is a lumbar puncture?
A lumbar puncture involves extracting some of the fluid that surrounds your brain and spine (known as cerebrospinal fluid or CSF). It is sometimes referred to as a spinal tap.
Often, a lumbar puncture is done because doctors need to do some tests on the CSF to help them make a diagnosis. Doctors may look for changes in the fluid that could indicate infection or bleeding, or unusual or uncommon cells that could be a sign of a neurological disorder. They will also check the pressure of the CSF.
Less frequently, a lumbar puncture can be done as a means of treatment if a person has too much CSF, and the pressure of the fluid around the brain and spine is too high.
What happens before the procedure?
A lumbar puncture is likely to take 30 minutes to an hour, so you don’t usually have to stay in hospital overnight.
There is no need to stop eating and drinking before the procedure, and you should continue to take any medication as prescribed, unless you have been told otherwise by your doctor. If you are taking any medication to thin your blood (anticoagulants) it is important that you inform the hospital before your appointment.
An experienced doctor or specially trained nurse will carry out the lumbar puncture. When you arrive for your appointment, the doctor or nurse will explain what is going to happen during the procedure and can answer any questions that you have.
What happens during the procedure?
You will lie curled up on your side, with your knees pulled into your chest and your back lined up with the edge of the bed. Alternatively, the doctor or nurse may ask you to sit on the bed with your head and shoulders bent forward so that your back curves out.
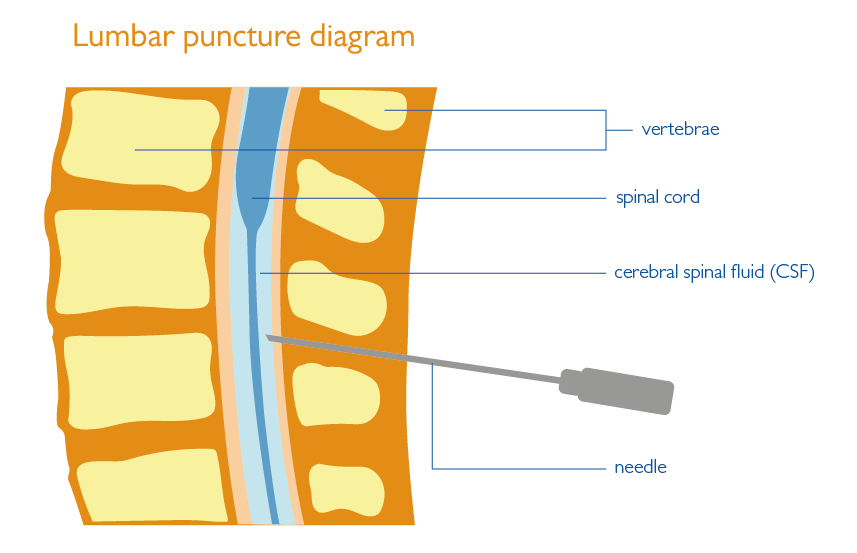
The doctor or nurse gives you a local anaesthetic injection into the lower part of your back where they will perform the lumbar puncture (“lumbar” refers to the lower back). This numbs the area. Then they insert a very thin needle between two vertebrae (spinal bones) at the base of your back and through the membrane (a thin skin-like layer) that surrounds the spinal cord and contains the CSF. This shouldn’t hurt but you may feel some pressure as the needle is inserted. Sometimes, a special x-ray or ultrasound may be used to help the doctor or nurse guide the needle into the right place.
Once the needle is in position, the pressure of the CSF is measured and some fluid is collected through the needle. The amount of CSF taken will depend on whether you are undergoing the procedure for the purpose of an investigation or a treatment. It may be necessary to remove more fluid if the lumbar puncture is being done as treatment for a condition.
A lumbar puncture is most often described as uncomfortable. The local anaesthetic injection should prevent you from finding the procedure painful. There is a chance you may feel a sudden sharp pain in one of your legs if the needle touches a nerve in your spinal column. The doctor or nurse will immediately adjust the position of the needle if this happens.
Once enough CSF has been taken, the needle is carefully removed and a plaster is put over the puncture site. You can remove the plaster the following day.
What happens after the procedure?
Immediately after the procedure, you will be advised to lie flat for an hour or so.
Usually, you can go home on the same day, but you should rest and avoid strenuous (very tiring) activity, as well as too much bending, lifting, stretching or straining. You should not drive yourself home following a lumbar puncture, so it is a good idea to make other arrangements for getting to and from your appointment.
A number of people experience headaches after having a lumbar puncture. This is a common side effect. It is caused by the drop in pressure around the brain that happens when the membrane is punctured and fluid is removed. The body will naturally replace the lost fluid but, in the meantime and while the membrane heals, it is a good idea to keep well-hydrated by drinking plenty of fluids. You may also take simple painkillers to help relieve the pain. Some people find drinks containing caffeine (such as coffee, tea or cola) can help to ease headaches, as can lying down completely flat for a time.
If you do experience headaches following the procedure, they should usually improve within a few days. A very small number of people, however, may experience headaches that persist and are sometimes accompanied by nausea (feeling sick) and/or vomiting. If this happens to you, you should contact the hospital.
Some people can experience backache following a lumbar puncture. The pain is usually mild and can be treated effectively with painkillers. Any backache should ease within a few days.
When will I know the results?
If you are having a lumbar puncture done for the purpose of a test, it is possible for results to be available in as little as a few hours in emergencies. However, you may have to wait for several days or weeks if more specialised tests are being done on the samples.
Thank you
We would like to thank everyone who contributed to this page, especially Samantha Colhoun (Clinical Nurse Specialist).
You can print this page by clicking the button below.
About this page
This fact sheet provides information on lumbar punctures. Our fact sheets are designed as general introductions to each subject and are intended to be concise. Each person is affected differently by encephalitis and you should speak with your doctor or specialist for individual advice.